Pregnancy is an extraordinary and transformative period in a woman’s life, marked by the anticipation of new beginnings and the joy of bringing life into the world. However, amidst the excitement, it’s essential to recognize the intricate physiological changes that occur within the body, including the often-overlooked impact on vascular veins. As hormonal fluctuations, increased blood volume, and the pressure exerted by the growing uterus create a unique environment, women may find themselves facing vascular vein issues during pregnancy.
In this comprehensive guide, we will navigate the intricacies of pregnancy and vascular veins, shedding light on what to expect and offering practical insights on effective management strategies. From understanding the physiological changes to adopting lifestyle adjustments, this guide aims to empower expectant mothers with the knowledge to navigate the challenges associated with vascular vein issues during this transformative journey.
Understanding Vascular Veins
Before delving into the specific impact of pregnancy on vascular veins, it’s crucial to have a basic understanding of the vascular system in such sitation every women should consult a varicose veins doctor. Veins are responsible for carrying blood back to the heart, and they often have valves that prevent the backward flow of blood. When these valves weaken or fail, blood can pool in the veins, leading to the development of varicose veins or spider veins.
Pregnancy and Vascular Veins
1. Hormonal Changes
Hormonal fluctuations are a hallmark of pregnancy. The increased production of hormones like progesterone can contribute to the relaxation of vein walls, making them more prone to dilation. This hormonal influence, combined with the pressure exerted by the growing uterus, creates an environment conducive to the development of vascular vein issues.
2. Increased Blood Volume
During pregnancy, a woman’s blood volume increases to support the growing fetus. While this is a natural and necessary adaptation, it can also put additional stress on the veins, potentially leading to the formation or worsening of vascular vein conditions.
3. Pressure on Pelvic Veins
As the uterus expands to accommodate the growing baby, it can exert increased pressure on the pelvic veins. This pressure may hinder the smooth flow of blood from the lower part of the body back to the heart, contributing to the development of varicose veins, especially in the legs.
4. Family History and Pre-existing Conditions
A woman’s genetic predisposition to vascular vein issues plays a significant role in whether she will experience them during pregnancy. If there is a family history of varicose veins or if the woman has pre-existing vascular conditions, the likelihood of developing or exacerbating vein issues during pregnancy may be higher.
What to Expect
1. Varicose Veins
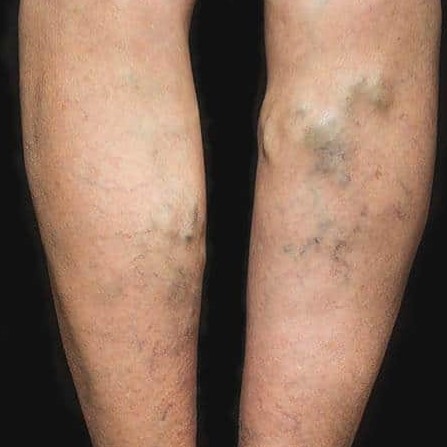
Varicose veins are enlarged, twisted veins that commonly occur in the legs during pregnancy. They may cause pain, swelling, and aching, especially after prolonged periods of standing or sitting. Varicose veins can be visually prominent, appearing as blue or purple bulging veins beneath the skin.
2. Spider Veins
Spider veins are smaller, red or blue veins that often resemble a spider’s web. While they are usually harmless, they can be aesthetically bothersome. Pregnancy can contribute to the development of spider veins, particularly in the legs.
3. Hemorrhoids
Hemorrhoids, swollen and inflamed veins in the rectum and anus, are another vascular issue that pregnant women may experience. The increased pressure on the pelvic veins can lead to the development or worsening of hemorrhoids, causing discomfort and pain.
Managing Vascular Vein Issues During Pregnancy
Managing vascular vein issues during pregnancy is a crucial aspect of ensuring the well-being and comfort of expectant mothers. The physiological changes associated with pregnancy, such as hormonal fluctuations and increased blood volume, can contribute to the development or exacerbation of vascular vein conditions like varicose veins and spider veins you must seek a guidance from vascular surgeon in Jaipur. Fortunately, there are practical steps and lifestyle adjustments that pregnant women can adopt to alleviate symptoms and promote better vascular health. From incorporating regular exercise and wearing compression stockings to maintaining a healthy diet and consulting healthcare providers, a proactive approach can make a significant difference. In this section, we will explore effective strategies for managing vascular vein issues during pregnancy, providing practical guidance to enhance the overall pregnancy experience.
1. Regular Exercise
Engaging in regular, low-impact exercises can help improve blood circulation and reduce the risk of developing or worsening vascular vein issues. Activities such as walking, swimming, and prenatal yoga can be beneficial. However, it’s crucial to consult with a healthcare provider before starting any exercise routine during pregnancy.
2. Leg Elevation
Elevating the legs whenever possible helps to reduce swelling and alleviate pressure on the veins. Keeping the legs elevated when sitting or lying down can promote better blood circulation.
3. Compression Stockings
Compression stockings are specially designed to provide graduated pressure, helping to improve blood flow in the legs. Wearing compression stockings, especially during periods of prolonged standing or sitting, can significantly reduce the discomfort associated with varicose veins.
4. Healthy Diet
A well-balanced diet that includes high-fiber foods can contribute to healthy digestion and prevent constipation, reducing the likelihood of developing or aggravating hemorrhoids. Adequate hydration is also essential for maintaining overall vascular health.
5. Avoid Prolonged Standing or Sitting
Prolonged periods of standing or sitting can increase pressure on the veins. Taking breaks to walk around and change positions can help alleviate this pressure and promote better blood circulation.
6. Weight Management
Maintaining a healthy weight during pregnancy is important for overall well-being and can also contribute to reducing the strain on the vascular system. Excessive weight gain may exacerbate vascular vein issues.
7. Consulting with Healthcare Providers
Pregnant women experiencing significant discomfort or noticing unusual changes in their veins should consult with their healthcare providers. A healthcare professional can assess the severity of the vascular vein issues and recommend appropriate interventions or treatments.
Conclusion
Pregnancy brings about numerous changes in a woman’s body, and the vascular system is not exempt from these transformations. Understanding the potential impact of pregnancy on vascular veins and taking proactive steps to manage and alleviate these issues can contribute to a more comfortable and healthy pregnancy journey. By incorporating lifestyle adjustments, seeking guidance from healthcare providers, and prioritizing self-care, women can navigate the challenges associated with vascular vein issues during pregnancy with greater ease and confidence.
Also Read – Essential Women’s Health: Regular Gynaecologist Visits